Nao Medical verifies insurance at intake with Ajaia and Stedi
Nao Medical is a comprehensive medical care provider. They offer urgent care, primary care, mental health, and other specialty services across their New York clinics and virtually.
Before every visit, Nao's on-site staff need to know what a patient's insurance coverage is and what the patient owes – things like co-pays and deductibles. That information helps them complete patient intake and move the visit forward.
With their old insurance verification workflow, getting those answers used to take 15-20 minutes per patient.
The process was also complex. It varied based on payer and involved manual handoffs between on-site and remote back-office staff.
To better serve their patients, Nao needed a faster, more reliable way to verify insurance coverage and confirm patient responsibility at the point of care.
Enter Ajaia, a healthcare AI transformation firm. They help healthcare organizations integrate AI into clinical and administrative workflows, from patient communication tools to custom internal apps. Ajaia focuses on replacing fragmented workflows by embedding solutions directly into the systems teams already use.
In 3 days, Ajaia built a lightweight eligibility tool on top of Stedi's Real-Time Eligibility API that lets Nao's on-site staff run eligibility checks themselves in a couple of minutes without handoffs.
Challenge
Nao's previous eligibility workflow was complex and time-consuming.
Details like co-pay, deductible, primary care physician (PCP) assignment, and network status – whether a service was in- or out-of-network – weren't available at the point of service.
To confirm coverage, on-site staff had to chat with a back-office teammate. They would log into the related payer portal, look up the patient's insurance benefits, and relay the details back.
Each check took 15-20 minutes, during which patients waited. Every payer used a different portal, with different interfaces and response formats, so logging in and parsing results took time.
Solution
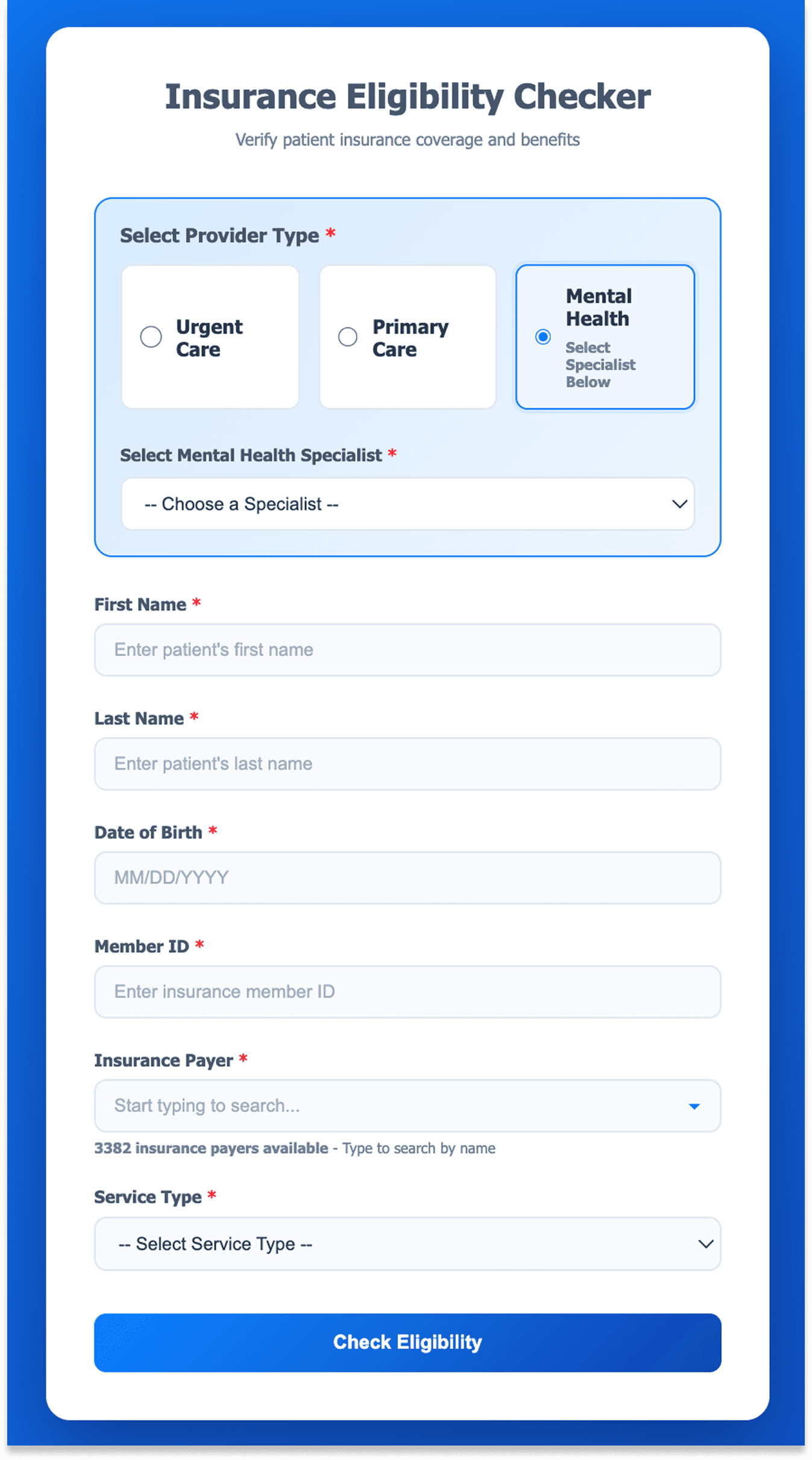
Ajaia's internal eligibility tool gives Nao's on-site staff a simple, user-friendly interface that works the same for every payer.
The eligibility tool was integrated into Nao's existing staff hub portals and internal systems, so on-site staff could run checks directly within the systems they already use without additional logins or process changes.
To check insurance, on-site staff only need to enter six fields: first name, last name, date of birth, member ID, insurance name, and service type.
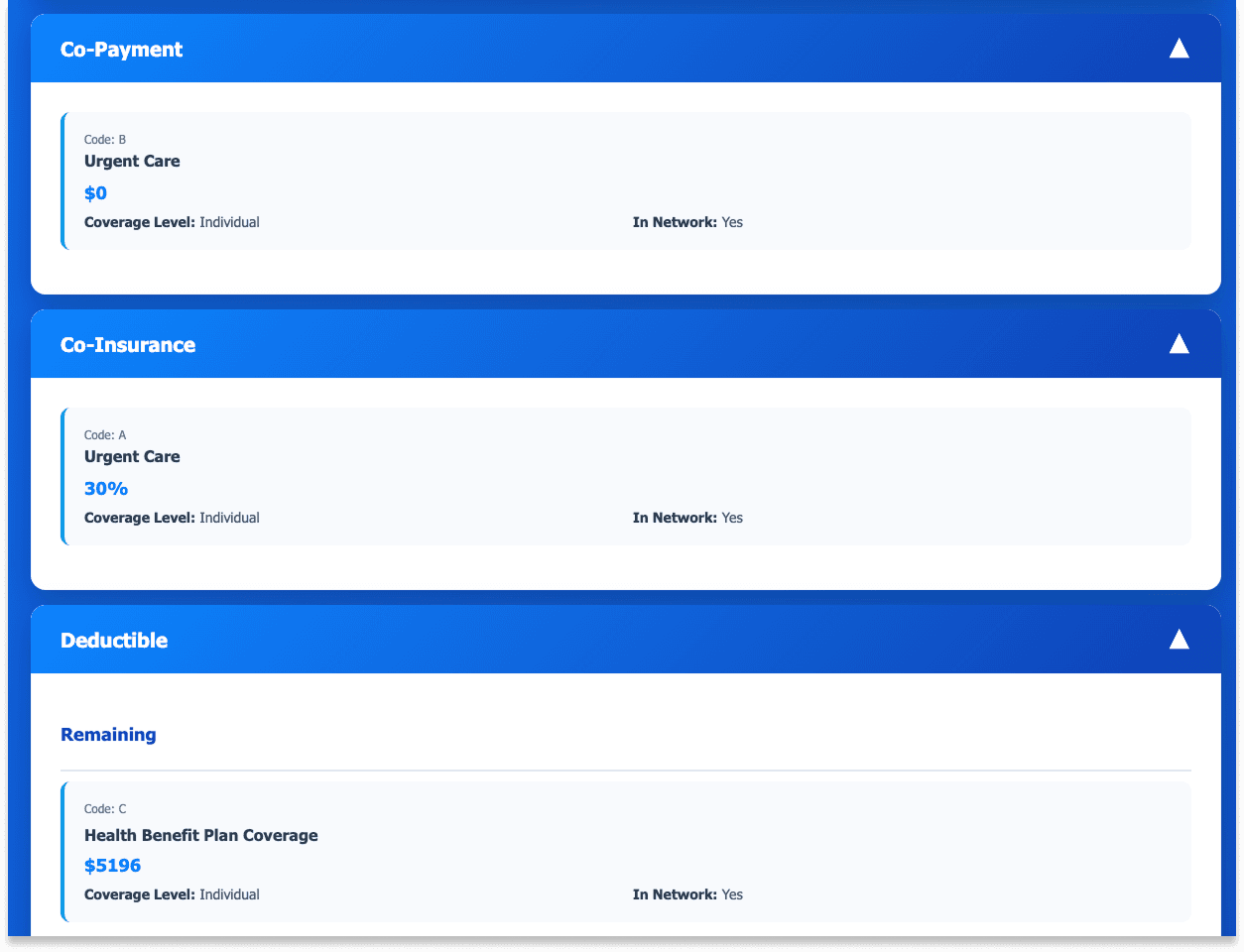
The tool provides accurate, structured answers in 1-2 minutes. The response includes every detail on-site staff need:
Co-pay amount
Deductible and out-of-pocket totals
PCP assignment and whether a PCP change is required
In- and out-of-network service details
The tool runs on Stedi's Real-Time Eligibility API, which returns responses in seconds in a consistent JSON format across payers.
At Nao, eligibility verification is now part of intake itself, not a decoupled back-and-forth workflow.
Results
A 15-20 minute handoff is now a 1-2 minute check, with responses in under a minute.
Nao's on-site staff no longer depend on a teammate to pull insurance details. They see what the patient owes, answer the patient's questions, and move the visit forward.
Ajaia didn't treat eligibility as a backend task. They built a workflow that matches how on-site staff actually work during intake – and shipped it in 3 days on Stedi's APIs.
Meet our customers and read the success stories from Stedi.
Automate healthcare transactions with developer-friendly APIs that support thousands of payers. Contact us to learn more and speak to the team.

