Run eligibility checks
You can run real-time 270/271 eligibility checks in your account to verify a patient's insurance coverage and benefits.
You can also run a special kind of real-time eligibility check called a Medicare Beneficiary Identifier (MBI) lookup. MBI lookups allow you to retrieve benefits information from the Centers for Medicare and Medicaid Services (CMS) when you don't know the patient's MBI.
Real-time eligibility checks
Real-time eligibility checks provide a response in seconds. They're ideal for in-person patient visits, telehealth appointments, and other scenarios where you need immediate information about a patient's coverage.
To run a new eligibility check:
-
Go to the Eligibility searches view.
-
Click + New eligibility check. Stedi opens the simplified eligibility check form, which we recommend for most use cases.
If you need to submit a check with additional information, click Swap to advanced form. On the advanced form, click Select fields on the top right of the window. The Select fields modal opens, where you can add additional form fields, such as the provider's Social Security Number (SSN) or procedure codes.
Check the boxes next to the fields you want to add to each section and click Save selection.
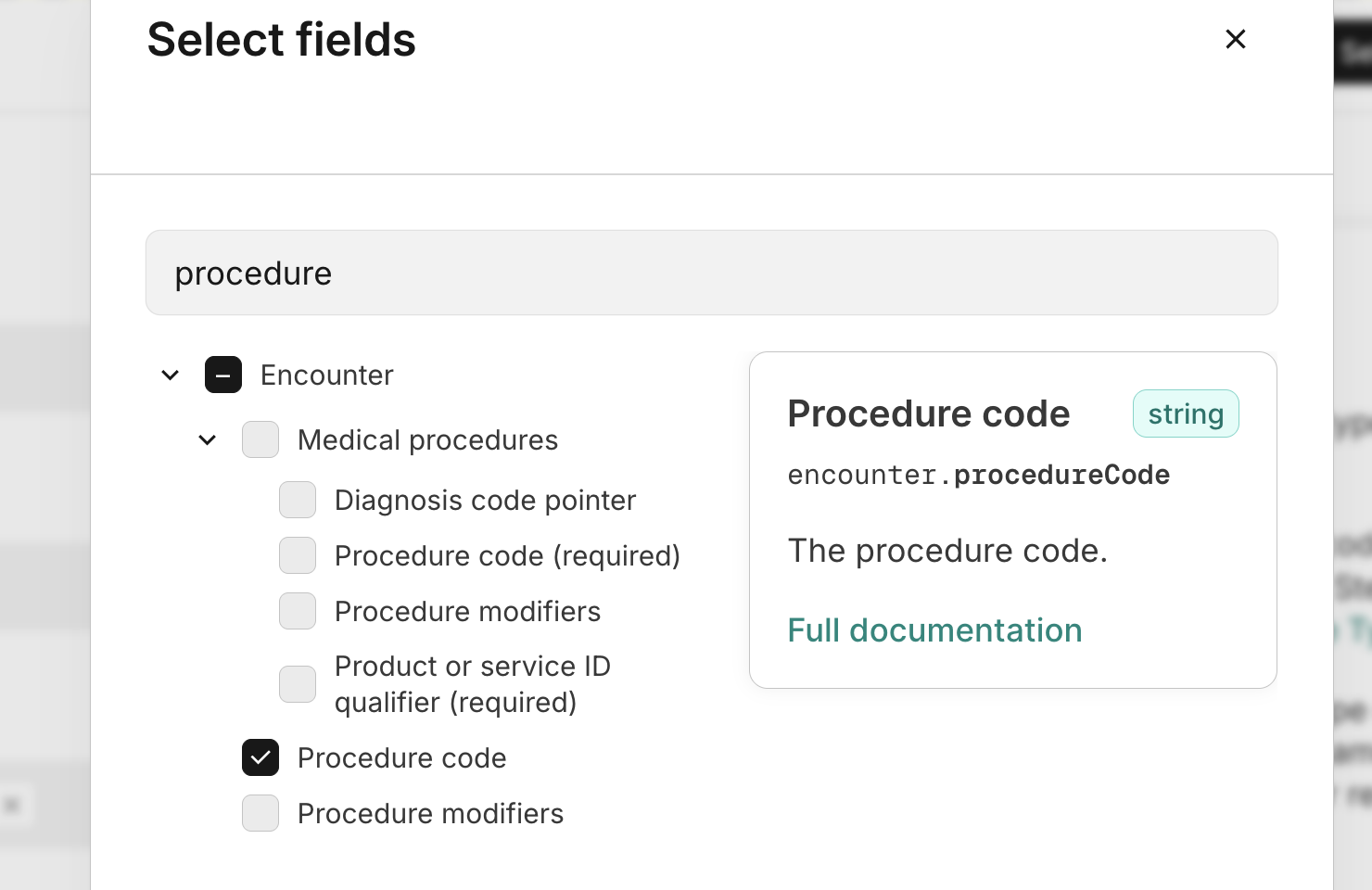
-
Complete the form. Review eligibility request fields for detailed instructions and tips for required fields. We especially recommend reviewing how to choose the right service type code (STC) or procedure code. This is very important for getting the best results from the payer.
-
Click Submit.
Stedi opens the Overview page for the eligibility check. If the check was successful, you can click Benefits to review the patient's benefits information.
If the check failed, you can review the error code and retry the check with updated information. Visit Fix failed eligibility checks for instructions.
MBI lookup
A Medicare Beneficiary Identifier (MBI) is a unique, randomly-generated identifier assigned to individuals enrolled in Medicare. You must include the patient's MBI in every eligibility check you submit to the Centers for Medicare and Medicaid Services (CMS).
When patients don't know their MBI, you can perform an MBI lookup instead of a standard eligibility check.
Types of MBI lookups
There are two types of MBI lookups you can perform with Stedi. For each, you'll use a special payer that tells Stedi to perform an MBI lookup for the patient in addition to a standard eligibility check.
| Type | What's required | Payer |
|---|---|---|
| With SSN | first name, last name, date of birth, Social Security Number (SSN) | CMS MBI Lookup |
| No SSN | first name, last name, date of birth, U.S. state | CMS MBI Lookup Without SSN |
We recommend running MBI lookups with the patient's SSN whenever possible. When the SSN is present, the MBI lookup has a higher likelihood of successfully returning their MBI. MBI lookups with no SSN are a fallback option when the patient's SSN isn't available.
You don't need to include more patient demographic information than what's required, such as additional address data. It doesn't improve MBI lookup success rates.
Run an MBI lookup
To run an MBI lookup:
-
Go to the Eligibility searches view and click + New eligibility check.
-
Click Swap to advanced form. The advanced form will allow you to add the additional fields required for an MBI lookup.
-
Construct an eligibility check request with the required patient demographic data. You don't need to include more than the required fields, such as extra address data. Extra demographic data won't improve lookup success rates.
-
With SSN: Include the patient's first name, last name, date of birth, and SSN.
You'll need to click Select fields and check the box next to Social Security Number (SSN) under the Subscriber section. This adds the SSN field to the form.
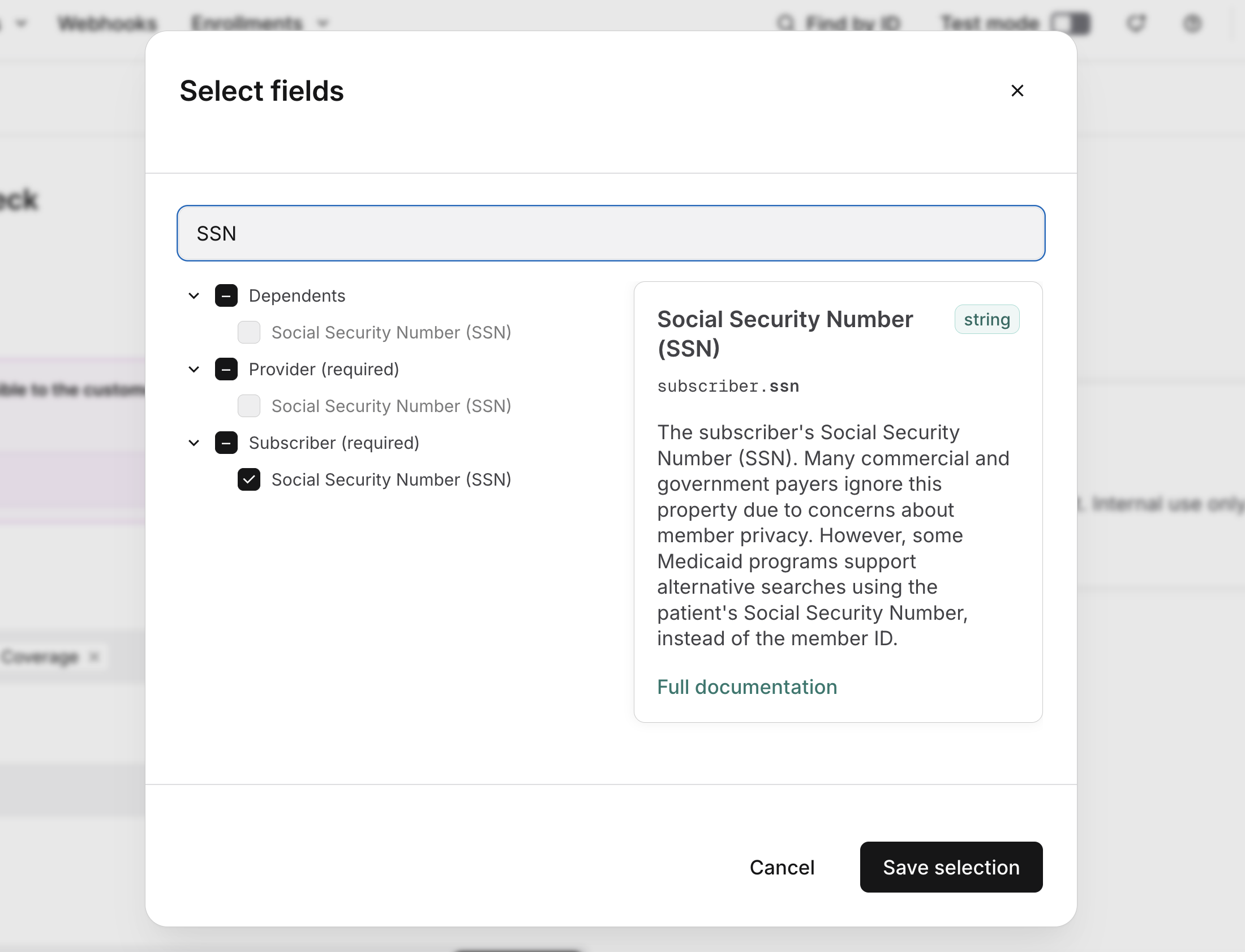
-
No SSN: Include the patient's first name, last name, date of birth, and U.S. state.
You'll need to click Select fields and check the box next to State under the Subscriber > Address section. This adds the State field to the form. You can leave the rest of the address fields blank.
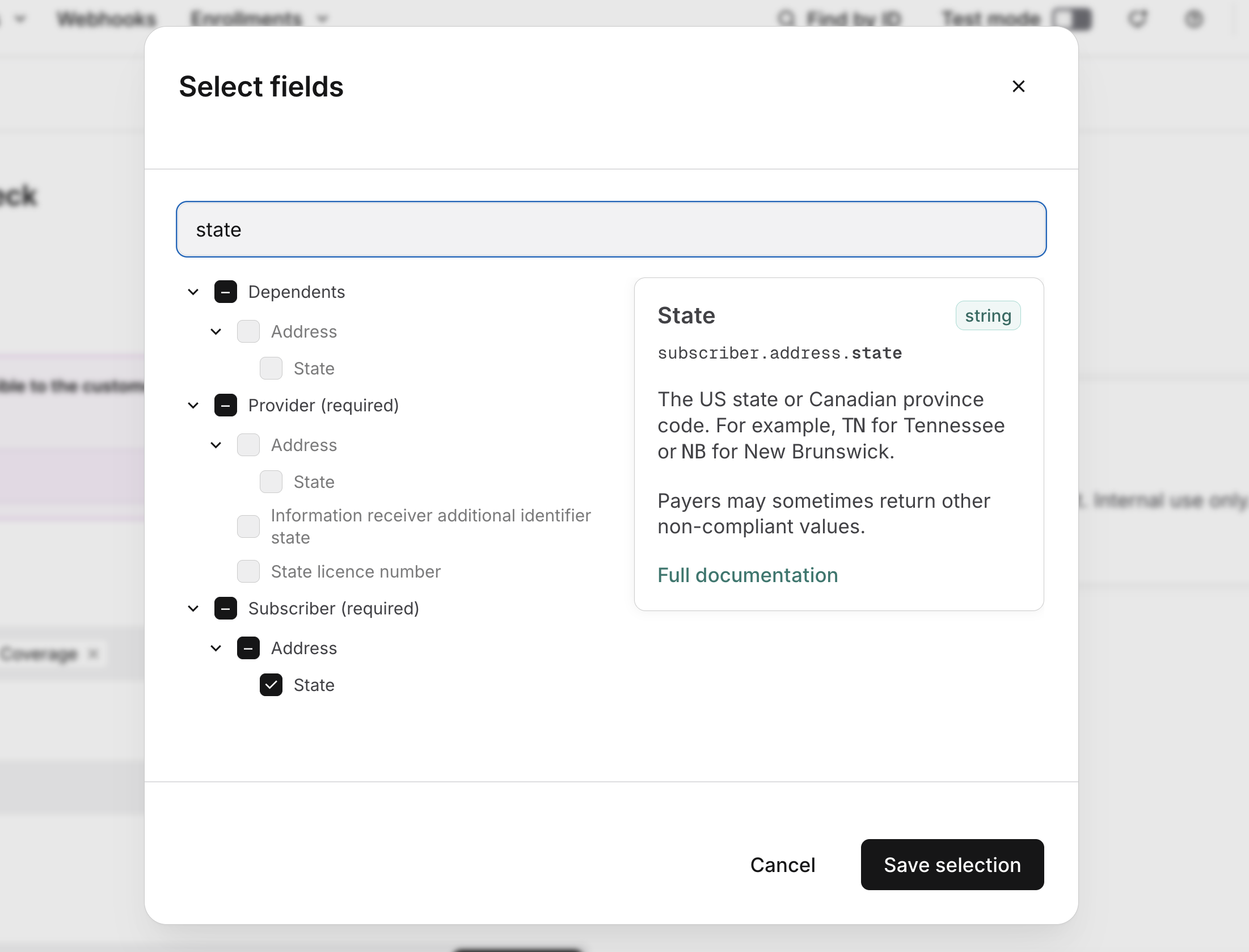
-
-
Set the Service type code to
30(Health Benefit Plan Coverage). -
Set the Trading partner service ID to either:
- CMS MBI Lookup for MBI lookups with SSN.
- CMS MBI Lookup Without SSN for MBI lookups without SSN.
-
Enter the rest of the required information. Review basic eligibility request fields for detailed instructions about how to complete remaining form fields.
-
Click Submit.
Stedi uses the patient's demographic data and SSN to perform an MBI lookup. If there is a match, Stedi submits an eligibility check to CMS. Stedi returns a complete eligibility response from CMS for the patient and returns the patient's MBI as the subscriber's member ID.
Stedi automatically opens the Eligibility search overview page for the MBI lookup when it's complete.
Medicare Advantage plans have their own unique member ID, which isn't returned in the MBI lookup response. You also shouldn't submit eligibility checks for Medicare Advantage plans to CMS (HETS) - you should submit them to the actual Medicare Advantage plan payer instead.
Outdated MBI error
Stedi's MBI lookup may rarely retrieve an outdated MBI for a patient. CMS may rotate an MBI for a member for various reasons at any time, such as to help protect against identity theft.
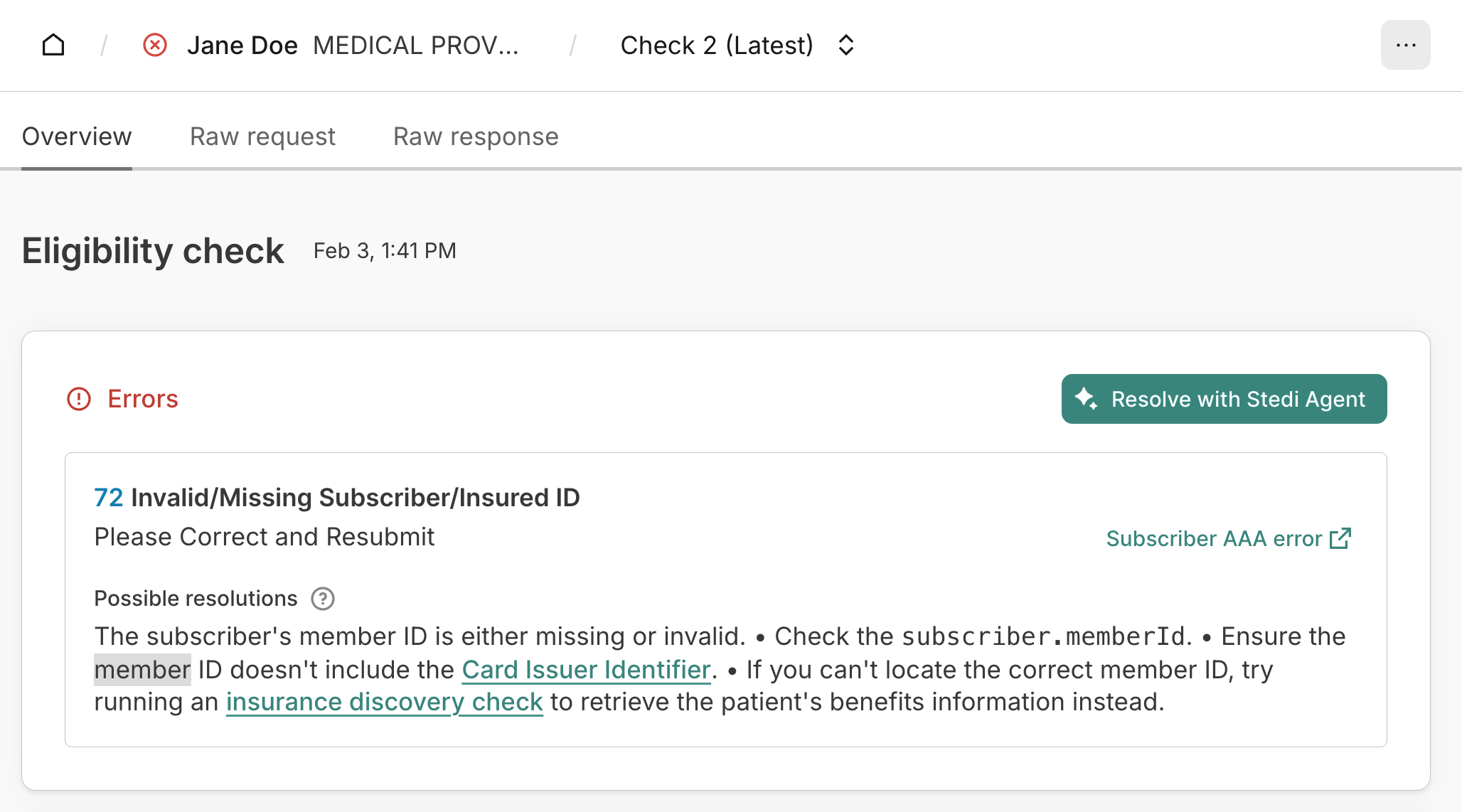
In these cases, the response will contain an AAA error with code 72 (Invalid/Missing Subscriber/Insured ID) and return a subscriber member ID, which is the outdated MBI.
Eligibility request fields
For the best chance of success, start by sending the smallest possible set of fields in your eligibility checks. Adding extra data can lead to unnecessary rejections.
We recommend starting with the following information. Only include more if the payer requires it.
| Form section | Instructions |
|---|---|
| Payer, or trading partner service ID | Select your payer from the provided list. Hover over view details to review a summary of the payer's various identifiers and open the full payer record in Stedi's Payer Network. |
| Provider | Most eligibility requests require the provider's name - either their first and last name (individual) or business name (organization) - and their National Provider Identifier (NPI). If you need to provide additional information, such as the provider's Social Security Number (SSN), click Swap to advanced form and then click Select fields to add additional fields to the request form. |
| Subscriber |
|
| Dependent | A patient qualifies as a dependent for eligibility checks when they are listed as a dependent on the subscriber's insurance plan and the payer cannot uniquely identify the patient through information outside the subscriber's policy. If the patient has their own member ID (even if it only differs by a suffix like 0), you must identify them in the Subscriber section instead.
|
| Encounter, service or procedure codes | You must include either a service type code (STC) or a procedure code and qualifier. This tells the payer what kinds of benefits information you're requesting. Most medical payers don't support procedure codes. Some dental payers do, but we recommend trying an STC first.
|
| Encounter, service dates | Stedi populates today's date as the date of service by default.
|
Patient information
Follow this guidance to help payers find the patient in their system.
Payer search requirements
All payers are required to be able to search for patients using the following "bare minimum" subsets of information. They will return benefits information as long as they can find a unique match for the patient within their system.
For a subscriber:
- Member ID, first name, last name, date of birth
- Member ID, last name, date of birth
- Member ID, first name, last name
For a dependent:
- Subscriber member ID, first name, last name, date of birth
- Subscriber member ID, last name, date of birth
- Subscriber member ID, first name, last name
Of course, not all of this patient information is always available. For example, a patient may forget their ID card. In these instances, some payers may still be able to search with even less information, such as the patient's first name, last name, and date of birth. Contact us if you have questions about alternative search options for a particular payer.
Dependents
The patient qualifies as a dependent for eligibility checks when:
- The patient is listed as a dependent on the subscriber's insurance plan.
- The payer cannot uniquely identify the patient through information outside the subscriber's policy.
When the patient meets these criteria, you should submit their information in the Dependent section of the form. Otherwise, you must submit their information in the Subscriber section instead.
For example, if the dependent has their own member ID number in the payer's database, you must identify them as a subscriber. This includes member IDs that differ only by a suffix, such as 01, because the patient can still be uniquely identified.
Medicaid dependents
Most Medicaid plans don't support dependents. However, some state Medicaid plans support eligibility inquiries for newborn children under 12 months old.
Children typically must be enrolled in Medicaid as a separate subscriber with their own unique member ID, even if they are legally the dependent of a parent who is a Medicaid plan member. Therefore, you'll almost always need to submit the child as a subscriber in the Subscriber section.
Sending dependent information to payers that don't support dependents will either cause an error, or the payer may ignore the information and return results for the subscriber instead.
Patient names
Note the following information and best practices when entering patient names:
- Enter the name exactly as written on the patient's insurance ID card (if available), including any special or punctuation characters such as apostrophes, hyphens (dashes), or spaces. If the patient's insurance ID card isn't available, enter the name exactly as written on a government-issued ID card. If a government ID card isn't available, enter the name exactly as given by the patient.
- Don't include a name prefix, title, rank, honorific, or academic degree in any field. These include Mrs., Dr., Hon., and PhD.
- Don't include a suffix or generation such as Jr. or III in the First name or Last name field. Put it in the separate Suffix field instead. Payers are supposed to automatically parse suffixes out of the last name, but Stedi can't guarantee that all payers will do this correctly.
- You can populate a middle name (or names) or initial in the Middle name field, but most payers ignore it when searching for the patient.
- Case doesn't matter. For example, JANE is equivalent to Jane.
The following are supported for patient names:
- Compound last and first names separated by spaces or hyphens such as Jean‐Claude or Smith Jones
- Apostrophized or elided names such as O'Connor or D'Amore
- Numbers like 3, however this typically indicates a data entry error
Some payers may have more specific requirements or restrictions that we don't cover in our docs. If you're receiving errors for a specific payer, we recommend consulting that payer's documentation for eligibility checks for additional guidance.
CMS HETS Rules of Behavior
All parties involved in eligibility transactions sent to the Centers for Medicare & Medicaid Services (CMS) eligibility system, called HETS, must comply with the HETS Rules of Behavior. Compliance is also required under our terms.
Review the Rules of Behavior before sending eligibility checks to CMS.