Review and resubmit claims
You can review, revise, and resubmit claims in the Stedi portal. This includes professional claims you submitted through the portal as well as professional, dental, and institutional claims third-party vendors submitted through Stedi on your behalf.
You may need to resubmit claims for several reasons, including changes to the patient's coverage, errors in the original claim's information, or appealing a denied claim. You may also need to cancel duplicate claims or claims that were submitted in error.
Pre-adjudication vs. adjudication
When resubmitting claims, you need to know whether your claim is pre-adjudication or in adjudication.
| Stage | Definition | How you'll know |
|---|---|---|
| Pre-adjudication | The claim hasn't entered the payer's adjudication system. This includes claims the payer has received and then rejected based on front-end edits. |
|
| Adjudication | The claim has entered the payer's adjudication system. This includes claims that were rejected during adjudication, claims still in progress (for example, in Pending status), and claims that completed adjudication (resulting in an 835 ERA). |
|
The following diagram illustrates the claim submission lifecycle and the responses you can expect to receive at each stage.
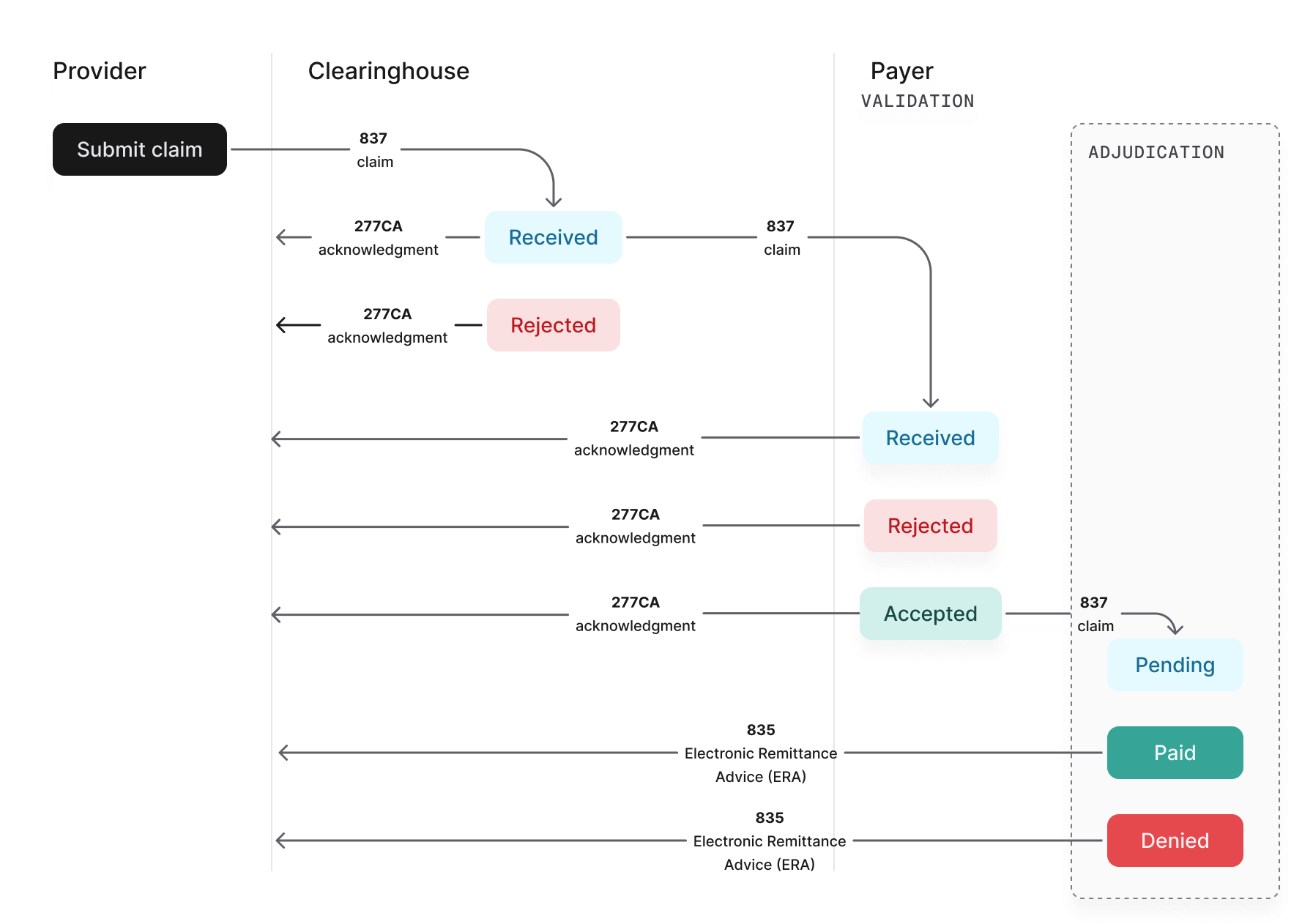
Preparing claim resubmissions or cancellations
Stedi's guidance for resubmissions varies depending on three factors:
- Whether the claim has entered the payer's adjudication system - Visit Pre-adjudication vs. adjudication to determine where your claim is in the lifecycle.
- Whether you're resubmitting to Medicare - Medicare Part A and Part B (processed through MACs) have different requirements than other payers. Visit Medicare resubmission for details.
- Claim type - Institutional claims have different requirements than professional or dental claims. Visit Institutional claims for details.
These factors determine which codes and identifiers to include in the resubmission:
- The proper Claim Frequency Code (CFC) - indicates the type of submission
- The Payer Claim Control Number (PCCN), if appropriate - the payer's unique identifier for your claim
- The appropriate Patient Control Number (PCN) - your unique identifier for the claim
You'll also need to include any necessary corrections to the claim data.
Claim Frequency Code (CFC)
The Claim Frequency Code (CFC) indicates the type of claim submission. It's what tells the payer the claim is an original, a replacement, or a cancellation.
| Scenario | CFC Guidance |
|---|---|
| Pre-adjudication (all payers) |
|
| Adjudication, non-Medicare |
|
| Adjudication, Medicare |
|
Set the CFC
You can set the Claim Frequency Code (CFC) in the following locations:
- X12 EDI:
Loop 2300 CLM05-03(Claim Frequency Code) component - CMS-1500 claim form UI: Set the Qualifier in Box 22 (Resubmission code)
Institutional claims
Institutional claims support a broader set of Claim Frequency Code (CFC) values than professional or dental claims.
For example, in long term care settings, facilities commonly submit interim claims every 30 days to receive partial payments while the patient is still admitted, rather than waiting until the end of the patient's stay. The CFC codes for these interim claims are 2 (Interim - First Claim), 3 (Interim - Continuing Claims), or 4 (Interim - Last Claim).
Therefore, the guidance for institutional claim CFCs is different from professional and dental claims. Specifically, for claims in pre-adjudication or Medicare claims in adjudication, you should resubmit with the same CFC you used in the original submission.
Payer Claim Control Number (PCCN)
The Payer Claim Control Number (PCCN) is the unique identifier the payer assigns when your claim enters their adjudication system. It's different from the Patient Control Number you sent in the original claim.
| Scenario | PCCN Guidance |
|---|---|
| Pre-adjudication (all payers) | Don't include a PCCN. The claim hasn't entered the payer's adjudication system yet, so no PCCN exists. |
| Adjudication, non-Medicare | Include the PCCN the payer returned in one or more responses to the original claim. Without the PCCN, the payer won't know which claim to replace or cancel. |
| Adjudication, Medicare | Don't include the PCCN. Medicare explicitly instructs providers to omit it when resubmitting claims. Visit Medicare resubmission for details. |
Set the PCCN
You can supply the Payer Claim Control Number (PCCN) in the following locations:
- X12 EDI:
Loop 2300 REF02, whereREF01=F8(Original Reference Number) - CMS-1500 claim form UI: Set the Original reference number in Box 22 (Resubmission code)
Find existing PCCN
You can retrieve the Payer Claim Control Number (PCCN) for the original claim from any of the following transactions from the payer.
| Transaction | How to get it |
|---|---|
| 277CA claim acknowledgment | Go to the claims view, click the claim to open its timeline, and click See more detail on the 277CA to review a user-friendly summary with the PCCN. |
| 277 real-time claim status | Run a claim status check for the claim you want to resubmit. The PCCN is available on the results page as Payer claim control number. |
| 835 Electronic Remittance Advice (ERA) | Go to the claims view, click 835 ERAs, and click the ERA to open it. On the Overview tab, the PCCN is in the Claims section in the Payer Claim Control Number column for each claim. |
Patient Control Number (PCN)
The Patient Control Number (PCN) is a unique identifier you assign to the claim. The payer returns this value in related transactions, such as the 277CA claim acknowledgment and 835 Electronic Remittance Advice (ERA), so you can correlate responses with the original claim.
| Scenario | PCN Guidance |
|---|---|
| Pre-adjudication (all payers) | Same PCN as original submission |
| Adjudication, Medicare | Same PCN as original submission |
| Adjudication, non-Medicare | New, unique PCN |
Reuse the same PCN from the original submission for pre-adjudication resubmissions and adjudication Medicare resubmissions. Stedi uses the PCN to match claims and resubmissions in the claims view, so reusing the PCN allows Stedi to show the original claim and resubmissions within a unified claim timeline. Reusing the PCN also helps you track the claim throughout the resubmission process.
Use a new, unique PCN for adjudication non-Medicare resubmissions. In this scenario, a new PCN helps you avoid potential duplicate claim errors from the payer. A new PCN also helps you differentiate between the 835 Electronic Remittance Advice (ERAs) for the original submission and the resubmission.
Set the PCN
You can set the PCN in the following locations:
- X12 EDI:
Loop 2300 CLM01(Patient Control Number) - CMS-1500 claim form UI: Set Box 26 (Patient account number)
PCN format
When assigning a PCN, follow these best practices:
- Use a unique PCN for each claim. The identifier should be more complex than a simple sequential number and should be hard to guess.
- Use random strings. Formats with patient initials or the date of service in them can create duplicates. We recommend using nanoid or a similar library configured with the characters available in the basic character set to create a strong, unique 17-character PCN for each claim.
- Keep it 17 characters or less. Some payers cut off values longer than 17 characters in ERAs and claim acknowledgments, which makes it hard to match them with the original claim.
- Use only characters available in the basic character set, and avoid special characters that are only available in the extended character set. Payers are permitted to return data using the basic character set. Using other characters may result in data loss or mismatches when correlating claims with responses.
- Treat PCN values as case-insensitive when matching transactions, even if the submitted value included both lower and uppercase characters.
Find specific claims
You can find a list of all your submitted claims on the claims view.
We recommend filtering for the claim's Patient control number (Loop 2300 CLM01) if it's unique for each claim. This will help you find the specific claim you're looking for. If you don't have the Patient Control Number, you can search for another identifier, such as the Patient name, to help narrow down the results. Your search terms must match what's in the claim exactly, including all spaces, capitalization, and punctuation.
Revise and resubmit claims
The resubmission process is the same for both corrections and cancellations - the Claim Frequency Code indicates which action you want to take.
- For professional claims, you can edit and resubmit through either the interactive CMS-1500 form or the X12 EDI editor.
- For dental and institutional claims, you can only edit and resubmit through the X12 EDI editor.
CMS-1500 form (professional)
Stedi's CMS-1500 claim form UI is mostly limited to the CMS-1500 form fields. It may not be able to successfully resubmit complex claims originally submitted through our APIs or SFTP.
To resubmit a professional claim through Stedi's interactive CMS-1500 form:
-
Go to the claims view and click the claim you want to resubmit to open its timeline.
-
Hover over the claim submission and do one of the following:
- Click Edit and resubmit. This option appears when the last claim submission was rejected by either Stedi or the payer.
- Click See more detail to review the claim's details page, then click Edit and resubmit.
-
Select CMS-1500 resubmission. Stedi opens the interactive CMS-1500 form prepopulated with the claim's information.
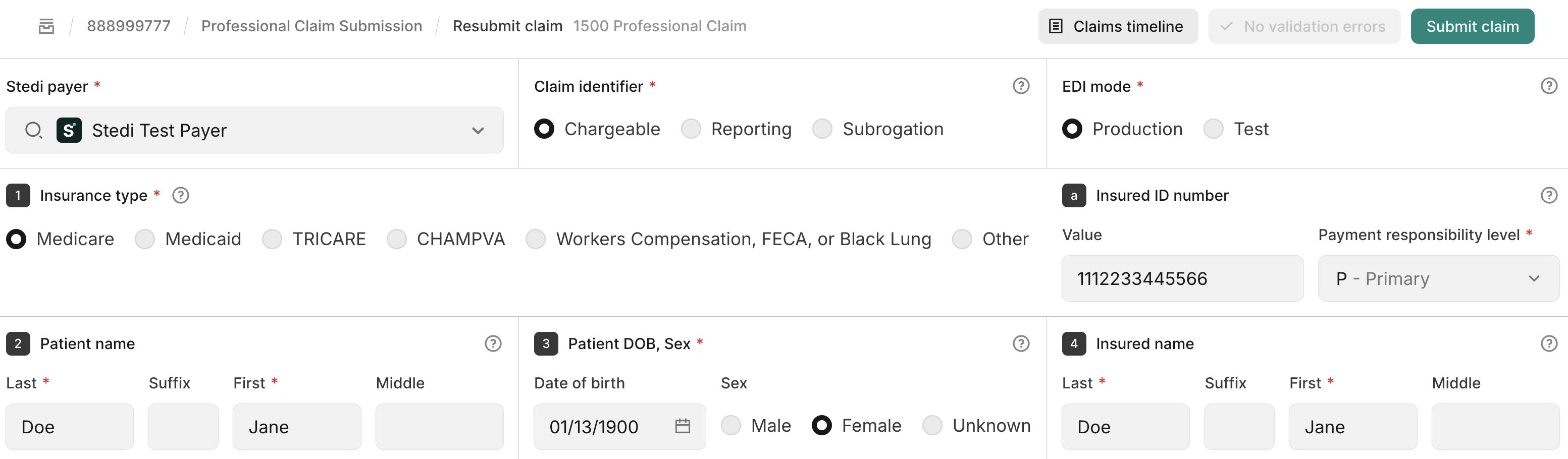
-
Make any necessary changes to the claim.
- Make sure to update the Claim Frequency Code, the Payer Claim Control Number, and the Patient Control Number according to best practices.
- Click Claims timeline to open a side panel with the claim's activity. You can review related 277CA claim acknowledgments containing the errors you need to address before resubmitting. Hover over a transaction and click See more detail to review its details.
-
Click Submit claim to resubmit the updated claim to the payer.
The updated claim will appear on the claims view within a few minutes. The claim timeline will reflect that this claim is a resubmission along with the original claim and any associated responses.
You'll receive new 277CA claim acknowledgments indicating whether the resubmitted claim was accepted or rejected.
X12 EDI editor
To resubmit a professional, dental, or institutional claim through Stedi's X12 EDI editor:
-
Go to the claims view and click the claim you want to resubmit to open its timeline.
-
Hover over the claim submission and do one of the following:
- Click Edit and resubmit. This option appears when the last claim submission was rejected by either Stedi or the payer.
- Click See more detail to review the claim's details page, then click Edit and resubmit.
-
Select X12 transaction resubmission. Stedi opens the claim in an interactive editor with the X12 EDI on the left and the EDI specification on the right.
As you hover over different parts of the EDI, Stedi highlights the corresponding part of the specification on the right to help you understand what each part of the EDI means and how to edit it correctly.
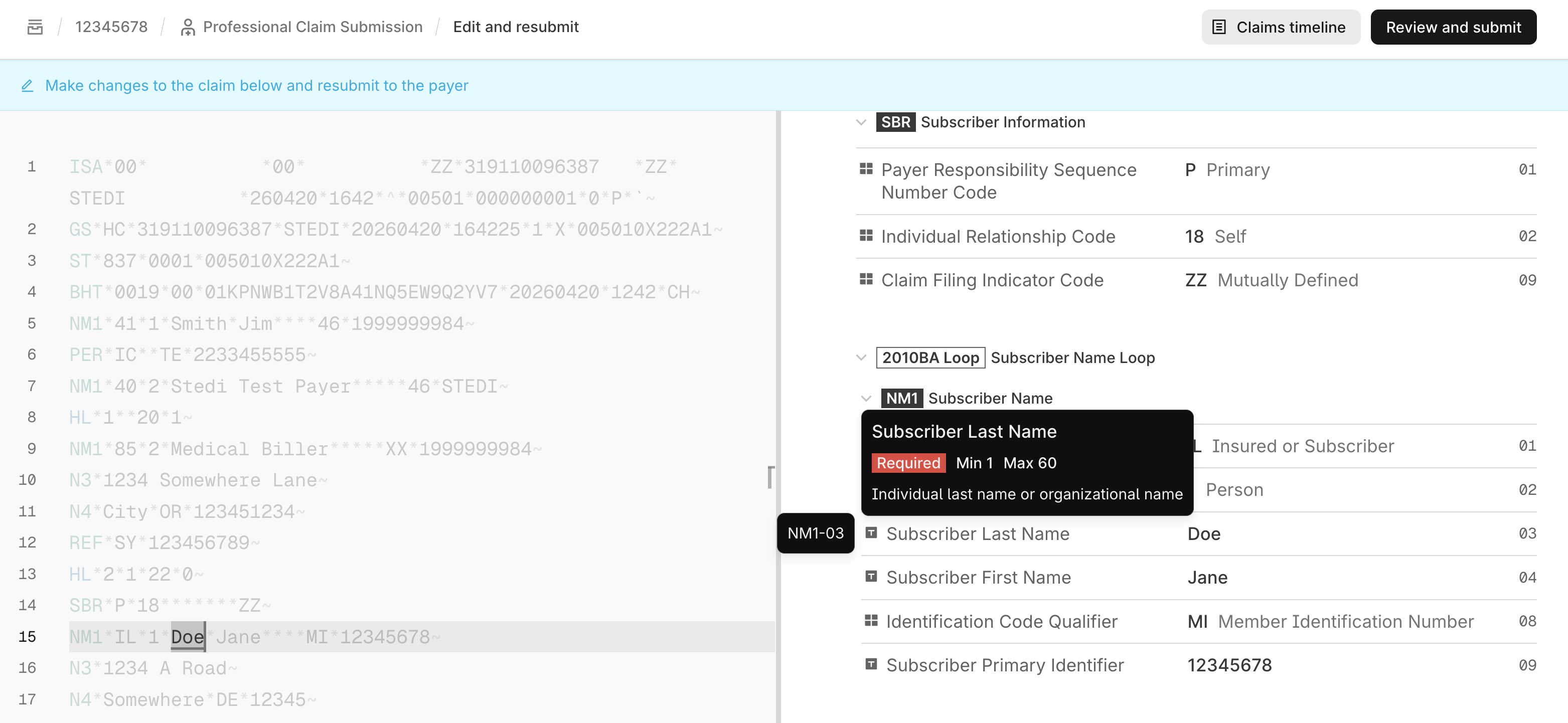
-
Make changes to the claim EDI.
- You can type directly in the EDI editor or copy and paste updated EDI from another source.
- Make sure to update the Claim Frequency Code, the Payer Claim Control Number, and the Patient Control Number according to best practices.
- Click Claims timeline to open a side panel with the claim's activity. You can review related 277CA claim acknowledgments containing the errors you need to address before resubmitting. Hover over a transaction and click See more detail to review its details.
-
Click Review and submit. Stedi shows a comparison of the original claim and the new claim containing your changes.
-
Click Resubmit claim to send the updated claim to the payer.
The updated claim will appear on the claims view within a few minutes. The claim timeline will reflect that this claim is a resubmission along with the original claim and any associated responses.
You'll receive new 277CA claim acknowledgments indicating whether the resubmitted claim was accepted or rejected.
Medicare resubmission
Medicare Part A and Part B (processed through MACs) have different requirements for resubmissions and cancellations than non-Medicare payers. Non-Medicare includes all other payers, such as commercial insurance and Medicaid.
- Medicare does not accept Claim Frequency Codes
7or8for resubmissions. For professional and dental claims, resubmit with Claim Frequency Code1. For institutional claims, resubmit with the same Claim Frequency Code as the original submission. - Don't include the original claim's Payer Claim Control Number (PCCN) when resubmitting, even if one is available.
Determine 277CA sender
To determine whether Stedi or the payer sent a 277CA claim acknowledgment:
- Go to the claims view.
- Find the associated claim and click it to view the claim timeline.
- Find the 277CA in the timeline view. The From field indicates whether the acknowledgment is from Stedi or the payer.
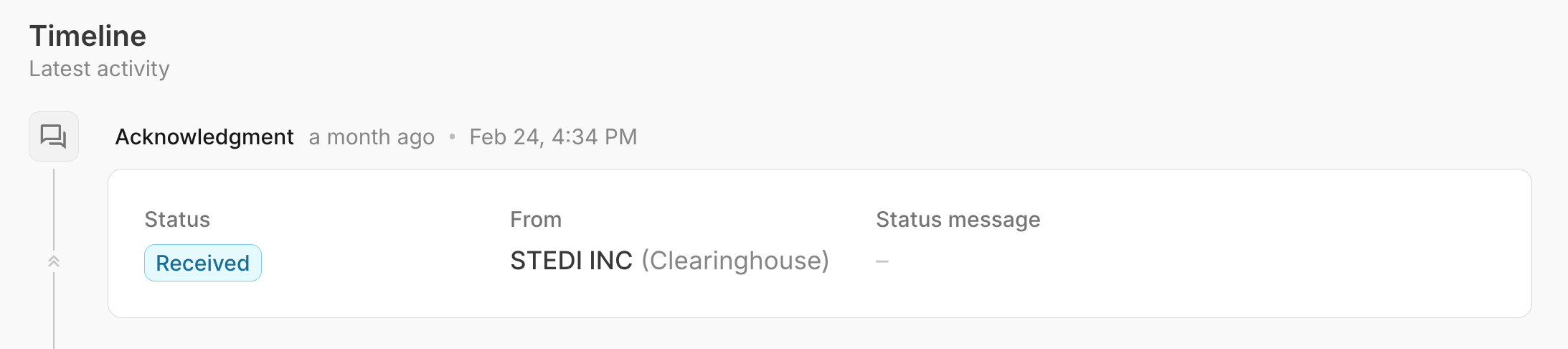
Character restrictions
Only use the X12 Basic and Extended character sets in request data. Using characters outside these sets may cause errors.
In addition, the following characters are reserved for delimiters in the final X12 EDI transaction to the payer: ~, *, : and ^. X12 doesn't support using escape sequences to represent delimiters or special characters. Stedi returns a 400 error if you use these restricted characters improperly.
- CMS-1500 form: Don't include delimiter characters anywhere in your request data.
- Raw X12: You can use these characters as delimiters, but not in the body of the request data.