Test claims workflow
You can submit test professional, dental, and institutional claims to make sure your claims process is working smoothly from end to end. When you submit test claims to the Stedi Test Payer, Stedi generates and returns an 835 Electronic Remittance Advice (ERA) based on the original claim.
Submit test claims
You can submit test claims with any payer ID and receive test 277CA claim acknowledgments from Stedi. This helps you test your claim submission workflow and practice interpreting and handling 277CA responses.
To send a test claim:
- In the 1500 claim form, select Test for the EDI mode.
- During X12 EDI upload, select Test from the dropdown at the top of the text area.
Stedi processes the claim and applies our entire catalog of edits and repairs.
Test 277CAs
When you submit a test claim to any payer, Stedi returns a test 277CA claim acknowledgment indicating whether the claim was successfully processed.
View test claims
When you designate a claim as test data, you can:
- View it in test mode from the claims view. Toggle test mode to ON to review test claims and their associated responses.
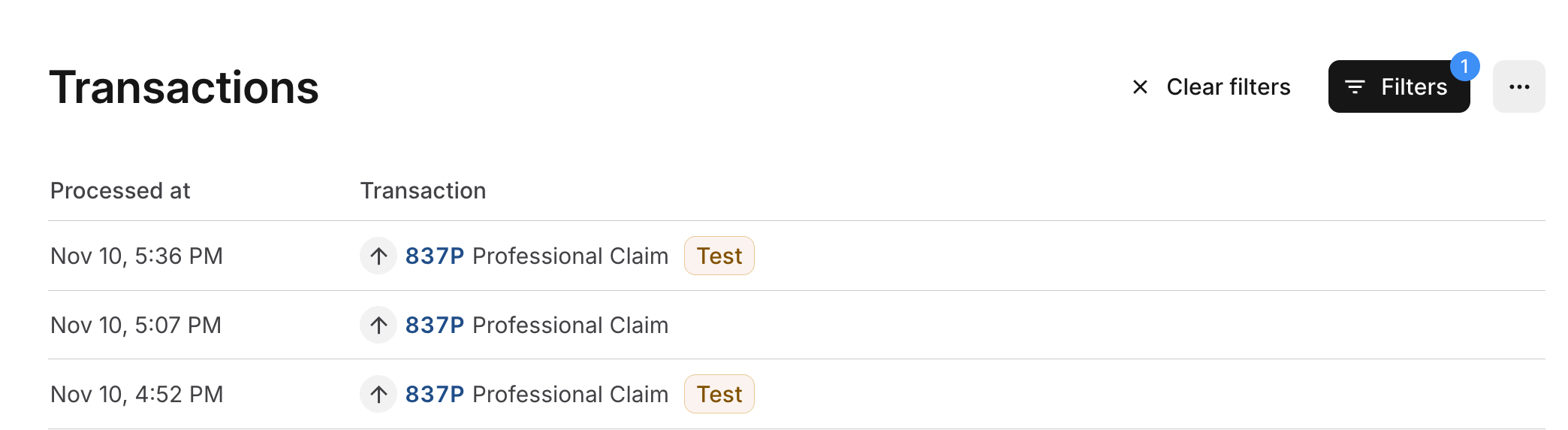
- Filter for test claims on the transactions view. The following example shows the Transactions page filtered to show only 837 claims. There are two test claims (indicated by the Test badge) and one production claim.
Generate test ERAs
When you submit test claims to the Stedi Test Payer, Stedi returns a test 277CA claim acknowledgment and a test 835 Electronic Remittance Advice (ERA) based on the original claim. Only test claims you send to the Stedi Test Payer will generate a test 835 ERA.
You can use this approach to test your claims processing workflow from end to end.
Enroll with the Stedi Test Payer
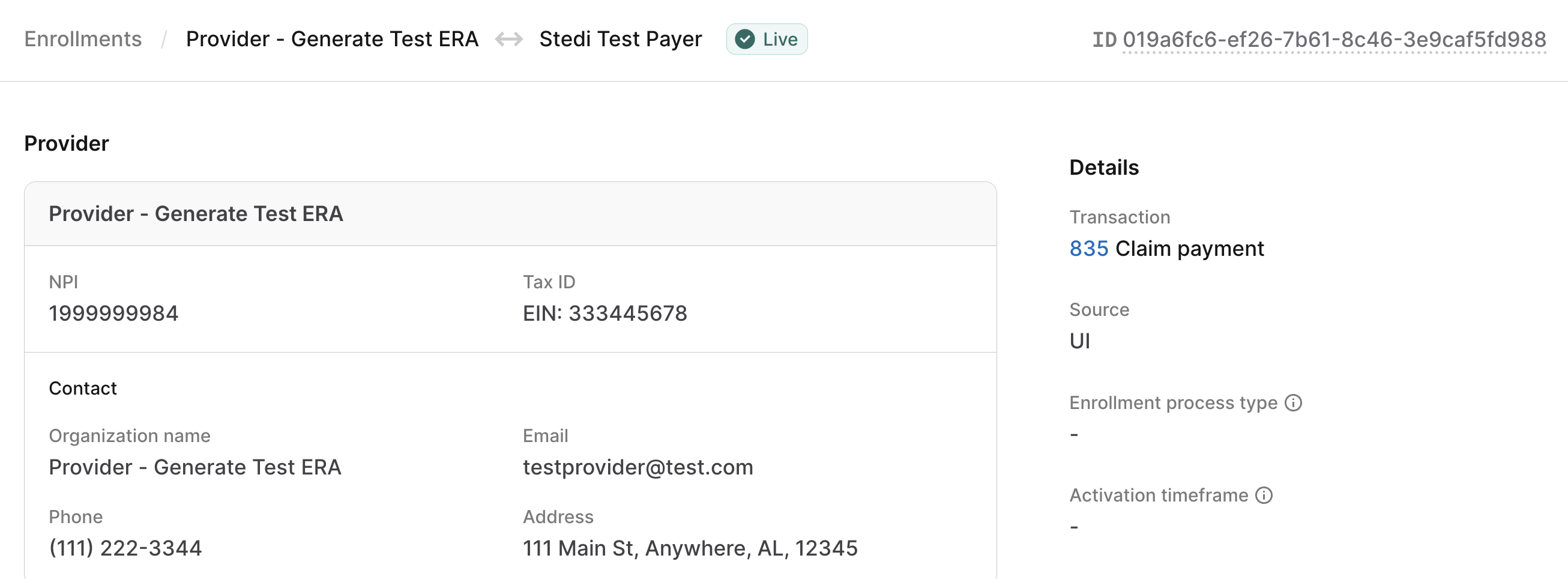
You must enroll your provider with the Stedi Test Payer for 835 Claim payment. Visit Transaction enrollment for instructions on how to submit an enrollment request.
Once submitted, the enrollment request is automatically set to LIVE status within one minute. You can start submitting test claims to the Stedi Test Payer immediately after enrollment.
Submit a test claim
Submit a test claim to the Stedi Test Payer. Ensure that you:
- Designate the claim as test data:
- Select Test for the EDI mode in the 1500 claim form.
- Set
ISA15(Interchange Usage Indicator) toT(Test Data) during X12 EDI upload.
- Set the payer to the Stedi Test Payer.
- Use the billing provider NPI and tax ID you enrolled with the Stedi Test Payer.
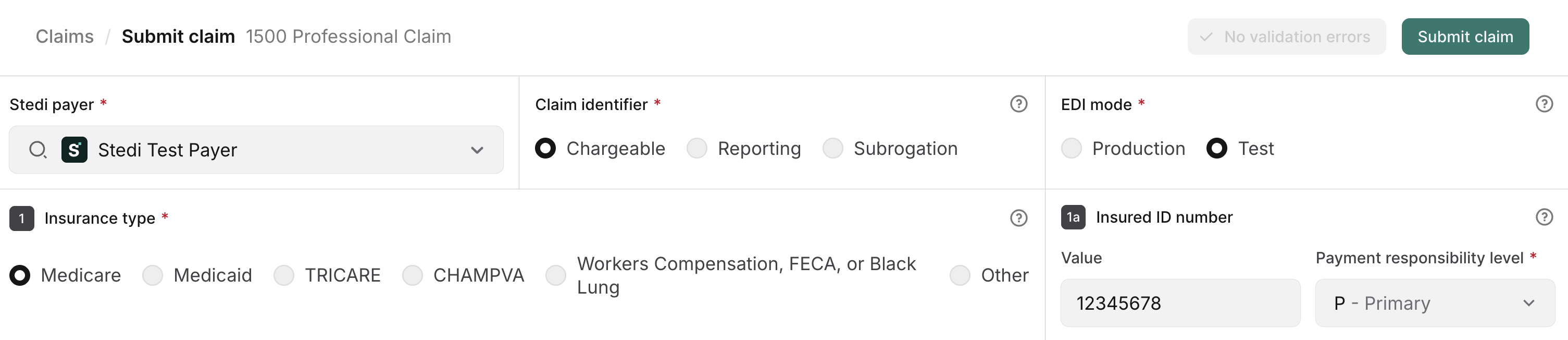
The following example shows how to submit a test professional claim to the Stedi Test Payer using the CMS-1500 claim form in the Stedi portal.
Test responses
Stedi returns the following responses within minutes of submitting a test claim to the Stedi Test Payer:
- A test 277CA claim acknowledgment response indicating whether the claim was successfully processed. Note that if Stedi rejects the claim in the 277CA, you won't receive a test 835 ERA.
- A test 835 Electronic Remittance Advice (ERA) containing information from the original claim, including the same:
- Provider information
- Patient information
- Service line details
- Charges
Test 835 ERAs always indicate that all service lines are paid, with the same charge amounts you submitted in the test claim. Note that when you submit real claims, payers may send ERAs with different outcomes, including partially paid, denied, split, or bundled claims.
Review test responses
You can review test 277CAs and 835 ERAs from the claims view in the Stedi portal. Toggle test mode to ON to view test claims and responses.
277CAs
Click All claims at the top of the page to view all test claims in your account.
- Click a claim to view a timeline of its processing activity.
- Click an Acknowledgment (277CA) to review its details.
Stedi displays key information about the 277CA, including the billing provider's information and status codes.
835 ERAs
Click 835 ERAs at the top of the page to review all test ERAs in your account.
- Filter by processed date, trace number, total paid, payment date, payment method, payer, payee (billing provider), payee NPI, payee Tax ID, or PCN (Patient Control Number).
- Click an ERA to review its details.
You can also find ERAs for a specific claim from the claim's timeline:
- Click All claims at the top of the page.
- Click a claim to view its timeline.
- Click Find matching ERAs in the side panel under the PCN to search for ERAs that match the claim's Patient Control Number (PCN). If no ERAs match, the ERA list will be empty.
- Click an ERA to review its details.
Both the test 277CA and the test 835 ERA will include the Patient Control Number you specified in the claim submission, which is what Stedi uses to match these responses to the original claim.
| Response type | How to find Patient Control Number |
|---|---|
| 277CA | On the Overview tab, the Patient Control Number is displayed as the Patient account number. |
| 835 ERA | On the Overview tab, the Patient Control Number is in the Claims section in the Patient Control Number column for each claim. |